The journey of starting a family can be a long and winding road. For some couples, the path to parenthood may involve the use of assisted reproductive technology like in vitro fertilization (IVF) and iui. In vitro fertilization (IVF) is a medical procedure in which a woman’s eggs are fertilized with a man’s sperm in a laboratory setting. IVF treatment is a complex process that requires the coordination of several steps to achieve success. In this guide, we will take a closer look at what is ivf, and steps involved in IVF treatment, and what people can expect during each stage of the process.
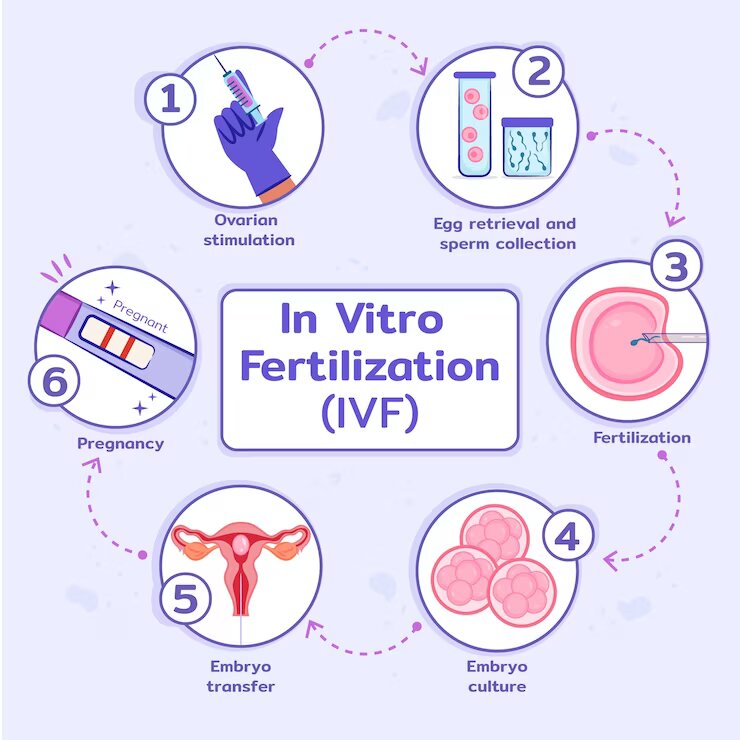
A Step-by-Step Guide to IVF Process
1. Ovarian Stimulation
Ovarian stimulation is a crucial part of the IVF cycle, as it increases the number of eggs that can be retrieved for fertilization. The goal of ovarian stimulation is to mature multiple eggs in the ovaries at the same time, increasing the success rate of fertilization and pregnancy. The most common hormones used for ovarian stimulation are gonadotropins, which are administered through subcutaneous IVF injection.
These medications work by stimulating the pituitary gland to release follicle-stimulating hormone (FSH) and luteinizing hormone (LH), which then stimulate the growth of the follicles in the ovaries. The most common gonadotropins are FSH-based medications such as Gonal-f, Follistim, and Menopur.
The ovarian stimulation protocol will vary depending on the mother’s situation, such as her age, the underlying cause of infertility, and her response to the medication. Typically, the stimulation begins on day 2 or 3 of the menstrual cycle and lasts for about 8-14 days. The patient will be closely monitored by a fertility specialist through blood tests and ultrasound scans to check the growth and maturity of the follicles, and the dosage of the fertility drugs will be adjusted as needed.
The monitoring is important because if the ovaries overreact to the medicines and produce too many follicles, it can lead to a condition called ovarian hyperstimulation syndrome (OHSS), which can cause symptoms such as abdominal pain, nausea, headaches, stress, bloating, and in severe cases, fluid accumulation in the lungs and abdomen.
Once the follicles have reached maturity, the patient will be given a trigger shot of human chorionic gonadotropin (hCG) to mature the eggs. The egg retrieval procedure is typically scheduled 36-38 hours after the trigger shot. It’s worth mentioning that some infertility clinics use a milder ovarian stimulation protocol called minimal stimulation IVF (Mini-IVF) or natural cycle IVF. This approach uses fewer medications and lower dosages, and it aims to retrieve one or two eggs with minimal stimulation.
2. Egg Retrieval
Egg retrieval is done through a procedure called transvaginal ultrasound aspiration, which is performed under conscious sedation. A thin ultrasound probe is inserted into the vagina and used to visualize the ovaries and the follicles containing the eggs. A needle attached to a suction device is then inserted through the vagina and guided to the ovary, where the eggs are collected. The procedure usually takes about 20-30 minutes and is generally well-tolerated.
During the procedure, the patient will be monitored by the doctor for any signs of discomfort or complications, such as bleeding or infection. The collected eggs are then transferred to a laboratory for fertilization. It’s important to note that the number of eggs collected can vary depending on the patient’s age, the underlying cause of infertility, structure, and the response to the ovarian stimulation medication. However, in general, the more eggs collected, the higher the chance of fertilization and pregnancy.
3. Sperm Collection
The sperm collection is usually done in a private room in the clinic or lab, where the men will be asked to provide a semen sample by masturbating into a sterile container. The sperm collection in the process of the treatment cycle takes about 15-30 minutes, and the sample is then immediately taken to the team for processing.
The laboratory will process the semen sample to separate the sperm from the semen, and then prepare the sperm for fertilization. This process, called sperm washing or sperm preparation, removes any debris or inactive sperm, leaving the healthy, motile sperm that will be used for fertilization. Sperm washing includes different techniques such as density gradient centrifugation, swim-up, and Percoll. Depending on the sperm quality and quantity, the embryologist will choose the most appropriate method.
Sperm quality and quantity can vary depending on factors such as the male partners’ age, overall health, and any underlying medical conditions. If there are issues with sperm quality or quantity, a technique called intracytoplasmic sperm injection (ICSI) may be used, in which a single sperm is directly injected into an egg.
4. Fertilization
There are two main methods of fertilization: intrauterine insemination and intracytoplasmic sperm injection (ICSI).
In insemination, the sperm and eggs are combined in a petri dish and allowed to fertilize naturally. The sperm will naturally migrate toward the egg, and if the sperm successfully penetrates the egg, fertilization will occur. Insemination is typically used when the sperm quality is good and the expected fertilization rate is high.
On the other hand, ICSI is a more complex technique in which a single sperm is directly injected into an egg using a small glass needle. ICSI is typically used when there are issues with sperm quality or quantity, or if previous IVF attempts have failed.
After fertilization, the resulting embryos will be observed for signs of normal development, such as the formation of the blastomeres and the formation of the inner cell mass. The embryologist will also grade the embryos based on their appearance and the likelihood of them leading to a successful pregnancy. The embryos will then be kept in a culture medium and will be observed for 2-6 days to check their development.
5. Embryo Transfer
The embryos are carefully selected based on their development and quality before being transferred into the woman’s uterus. The transfer itself is a relatively simple procedure that is typically performed in a clinic or hospital. The woman will lie down on an examination table and a thin, flexible catheter is inserted through the cervix and into the uterus. The embryos are then gently pushed through the catheter and into the uterus.
The procedure usually takes only a few minutes and the woman can go home shortly after. It is usually painless, but some mild cramping or discomfort may be experienced. It’s important to note that after the transfer, the woman should avoid some activities for a few days, and also avoid intercourse for about a week.
6. Luteal Phase Support
Luteal phase Support is a treatment that is given to women undergoing IVF treatments to support the development of the uterus lining after the embryo transfer. It is used to supplement the hormones that are naturally produced by the body during this phase to ensure that the uterus is properly prepared for the implanted embryo.
Progesterone is the main hormone used for luteal phase support, which is usually given as an injection for infertility treatment. It can be started after the embryo transfer and continued until the pregnancy test which is usually 2 weeks after the transfer.
7. Pregnancy Test
A pregnancy test is done 14 days after the embryo transfer to check if the treatment has been successful. The most common type of pregnancy test is a blood test, which measures the levels of a hormone called human chorionic gonadotropin (hCG) in the woman’s blood. This hormone is produced by the placenta shortly after the embryo implants in the uterus. The blood test is more sensitive than a urine test and can detect lower levels of hCG, making it more accurate in detecting early pregnancies.
Conclusion
The procedure of IVF pregnancy can be a rollercoaster of emotions and risks, from the excitement of the ovarian stimulation to the anticipation of the pregnancy test. It’s important to remember that while fertility treatments are not a guarantee of pregnancy, it is a powerful technology that can increase the chances of couples achieving their dream of starting a family. It gives hope to couples. The process may be long and challenging, but the result of holding a newborn baby in your arms makes it all worth it. So talk to your partner, decide to choose the best fertility clinic, and take doctors’ advice.
Frequently Asked Questions:
How Long Does the IVF Process Take?
Normally, the entire IVF process can take 3-6 months, although some patients may require additional time in IVF progress.
How Much Does the IVF Process Cost?
Depending on the particular circumstances of each patient, the cost of in vitro fertilization (IVF) can vary significantly.
How Many Cycles of IVF Will I Need?
The number of IVF cycles depends on a variety of factors, including age, medical history, and the cause of infertility.

