It’s more normal than it used to freeze your eggs to put off getting pregnant. If you choose to freeze your eggs, you can take care of other things in your life until you’re ready to get pregnant. This is helpful if you want to start a job, find a partner, or deal with health issues.
People don’t think twice about freezing eggs anymore, but not everyone knows the whole process. To make an informed choice, you need to know what to expect, how much it will cost, and how egg saving can help you stay fertile.
How do you Freeze Eggs?
When eggs are frozen, they can be used in assisted reproductive technology (ART). This is also known as embryo cryopreservation.
Medications are used to help the eggs grow during the process. The eggs are then taken out of the ovaries and frozen to keep them safe. The eggs can be warmed and mixed with sperm at a later time to make a baby. During the embryo transfer stage, the egg can then be put into the uterus.
Some people choose to freeze their eggs so that they can be used later. Freezing eggs is also done by people who donate them so that someone else can use them during fertility treatments.
No matter because you want to freeze eggs, the end goal is the same: keeping eggs lets you keep your fertility by collecting eggs at a younger age that can be used later. This won’t guarantee a pregnancy, but it can make it more likely that you’ll be able to get pregnant later in life.
How To Egg Freezing and When to Do It
You can expect the whole process of freezing eggs to take between 2 and 3 weeks, though exact times may change. It’s possible to finish most rounds in less than two weeks.
To get the best results, stimulating the ovaries to make eggs at the right time for you is timed with your period. Ultrasounds and blood tests to check hormone levels are used to carefully watch the ovaries during this process.
Medical Check-up
You will first need to talk to a fertility doctor about your plan to freeze your eggs. Your doctor will set up an appointment for an exam, during which they will look at your medical history, do blood work, and test your hormones.
A transvaginal ultrasound will also be used to do an antral follicle count (AFC). This is a way to measure your ovarian reserve or the number of eggs that are still in your ovaries.
During this time, your fertility doctor will talk to you about the best way to stimulate your ovaries so that you can safely get the most eggs without getting ovarian hyperstimulation syndrome (OHSS).
This is a reaction that can happen after a woman gets hormone shots during ovary stimulation.
Your doctor will also give you an idea of how many eggs they think they will be able to retrieve and tell you how to take the medicines that will trigger your ovaries and get them ready for retrieval.
Monitoring and Stimulating the Ovaries
Starting this process might involve taking birth control pills or other drugs like estrogen, lupron, or Aygestin, depending on what your doctor says and where you are in your menstrual cycle. These drugs will help your follicles get ready for the stimulation drugs you’ll be taking later.
If you receive instructions to take birth control or other medications that regulate your periods. You will usually start doing so during your period or right after you ovulate.
To make sure you start stimulation shots at the right time, you will still be checked on with either blood tests or ultrasounds. Once you’re given the all-clear to start shots, your doctor or treatment planner will give you clear advice on how to give yourself the injections.
Most people will take gonadotropins, which are hormones like follicle-stimulation hormone (FSH) and luteinizing hormone (LH). These hormones tell the ovaries to make more than one egg during a cycle.
It will take about 10 to 12 days of straight shots of these medicines under the skin in the belly. We closely monitor you during those days, and based on how your body responds to the injections, your doctor may adjust the dosage and combination of your medications.
From day 5 to day 7, your eggs may start to get bigger, so don’t be surprised if your doctor tells you not to do hard activities like running or high-impact workouts during this time.
Most of the time, you will have three to five tracking visits during the stimulation process to see how your follicles are doing. A trigger shot, which is an injection of medicine, is given once the follicles are big enough. The medicine is usually human chorionic gonadotropin (hCG), lupron, or a mix of the two.
Getting Egg Retrieval
Egg removal, which is also called egg picking, is the process of getting eggs out of your ovaries. As part of this process, you will go to your doctor’s office or clinic and be given an IV. This will let them give you general anesthesia for the surgery since you’ll be asleep during it.
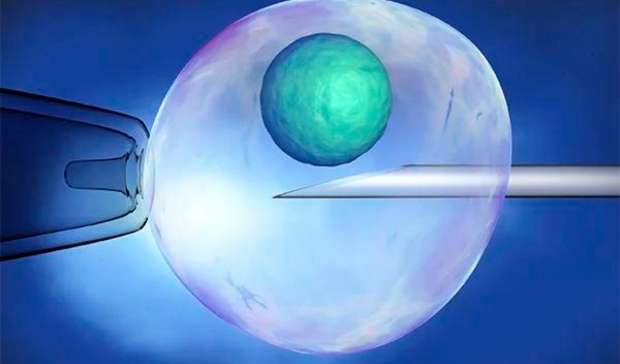
Your doctor will use a transvaginal ultrasound tool with a needle to get the eggs. The needle will be put into your follicles with the help of the ultrasound. The fluid that holds the eggs inside the follicles is sucked out and put into tubes, which are then given to an embryologist.
The embryologist will look at the follicle fluid to find the eggs. It takes about 10 to 20 minutes to finish the whole process. Your doctor will tell you how many eggs were taken out when you wake up.
A lot of things affect how many eggs are removed, but age and ovarian reserve are the two most important ones. People aged 40 and up tend to have fewer eggs taken than people younger than 35.
Getting Better Egg Freezing Process
In the 24 hours after egg removal, it’s normal to have cramps, bloating, constipation, and spotting in the pelvic area. Over-the-counter painkillers or warm pads can help most people feel better.
Call your doctor right away if you have more intense stomach pain, feel dizzy or faint, or have heavy vaginal blood.
Once we safely collect the developed eggs, we quickly freeze them using a process called vitrification. By rapidly freezing the eggs with liquid nitrogen, we reduce the chance of ice crystals forming and increase the number of eggs that survive.
Who Might Thinking About Egg Freezing Procedure
Egg freezing can serve many purposes, but the most common are delaying pregnancy, preserving fertility, or donating eggs.
Many people, especially those in their 20s or early 30s, choose to put off having children to advance their careers or for other reasons. Putting eggs in the freezer when you’re younger will help you get more babies if you ever need or want to use them.
On the other hand, people with serious health problems that could affect their ability to have children, like cancer, polycystic ovarian syndrome (PCOS), or endometriosis, may be told to freeze their eggs before starting treatment to keep their fertility.
Also, people who were born with ovaries and want to change their gender and may start treatment like hormone therapy or surgery may freeze their eggs to keep their fertility for the future.
Risk And Side-Effects Of Egg-Freezing Process
The process involves some risks. Most people will only feel pain during the injections and right after the egg extraction. Ovarian hyperstimulation syndrome, or OHSS, can happen very rarely to a patient.
OHSS can happen when the medicines used to make the ovaries make more eggs also raise hormone levels very high. This can make the ovaries get bigger, fluid leaks into the belly, and chemical problems happen.
Researchers have found that this side effect is more likely to happen to people younger than 35. In the same way, people who already have diseases like PCOS or a low body mass index (BMI) may be more likely to get OHSS.
Also, keep in mind that changes in your hormones during a normal monthly cycle can affect your mood, and so can stimulant drugs. Freezing eggs can cause stress, which can get worse when you take hormone medicines.
Injections of hormones and stimulation of the ovaries can also cause skin soreness at the injection sites and ovarian torsion, a rare disease in which the ovary turns on itself and cuts off its blood supply. It can be really painful.
How Much Cost Consider Egg Freezing
Egg freezing costs a lot of different amounts, based on where you live and which center you go to. Know this: Most insurance plans won’t pay for this process unless your pregnancy is in danger because of a health problem like cancer.
We price egg freezing by cycles, which usually include the process of stimulating the eggs (we give them medicine and monitor their growth) until we remove and freeze them.
It can cost anywhere from $5,000 to $10,000 per cycle to freeze eggs. The total cost of the cycle may go up when you add in the cost of the medicines, which can be anywhere from $2,000 to $7,000 based on the amount and mix of medicines that are given.
You should also think about how much it will cost to store your eggs. The center determines the exact amount that this will cost each year, which may be $500 to $1,000.
If you want to freeze your eggs, look for centers that let you pay over time. You could also move to an insurance company that covers freezing eggs.
There are funding programs for fertility, like the Hope for Fertility Foundation, the Baby Quest Foundation, and the Cade Foundation.
People who want to freeze their eggs as a way to avoid having a health problem that could make them unable to have children should look into grant programs that are specifically for this purpose. Livestrong Fertility, the Heart Beat Programme, and Fertility Within Reach are all great choices.
What should you do to get ready to freeze eggs?
You might want to bring a partner, a trusted friend, or a family member with you on the day of your egg harvesting process. Wear clothes that are easy to move around in, and plan to relax right away after the process. It’s normal to need a few days to get over the pain of extraction.
Also, it helps to know what to expect. Prepare yourself for a small change in your life, at least while we freeze your eggs.
Watch what you eat and drink as little coffee and alcohol as possible. In the meantime, do what your doctor tells you to do, especially if they tell you to stay away from more intense things like sex or high-impact exercise.
You might feel a little more worried or have mood swings because of the drugs you’re taking. Take it easy and be kind to yourself.
Conclusion
Studies show that egg freezing helps people who want to maintain fertility, whether they worry about their health, want to delay having children or plan to change their gender. It might not be possible for everyone to afford it, but some programs can help lower the cost.
It takes a couple of weeks of treatment. The chance to keep your fertility can have many perks that make it worth it.
FAQs regarding the process of egg freezing
Is it painful to freeze an egg?
Do remember that you will be asleep during the process. However, it’s normal to feel some cramps, soreness, or aches right after the operation.
How old should you be to freeze your eggs?
Most women are most fertile when they are 30 years old (Source). Many factors determine what happens next, like the receiver’s age and the number and type of eggs they use.
Is there anything that could go wrong with a fetus that comes from a frozen egg?
There are no known risks for fetuses that grow from frozen eggs, as long as there are no underlying illnesses. But once you’ve put eggs and sperm together to make a baby, you can choose to do preimplantation genetic testing, or PGT, on it to check for chromosomal problems.
What are the chances of getting pregnant with frozen eggs?
Many factors determine what happens next, like the receiver’s age and the number and type of eggs they use.
If you are under 35 years old and freeze 20 eggs, one study found that you will have at least one live birth. People who freeze only 5 eggs are 5.9% less likely to have a live birth.